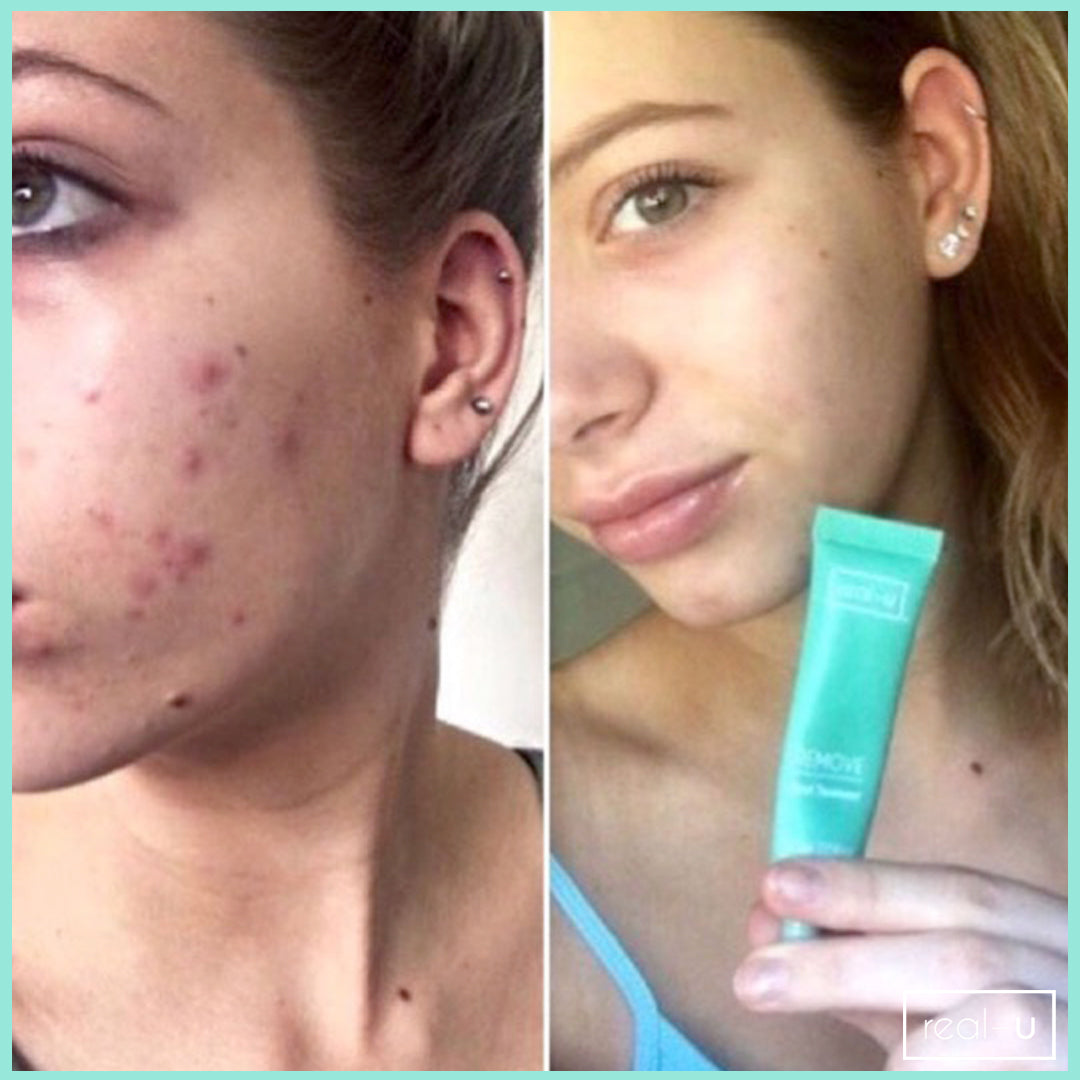
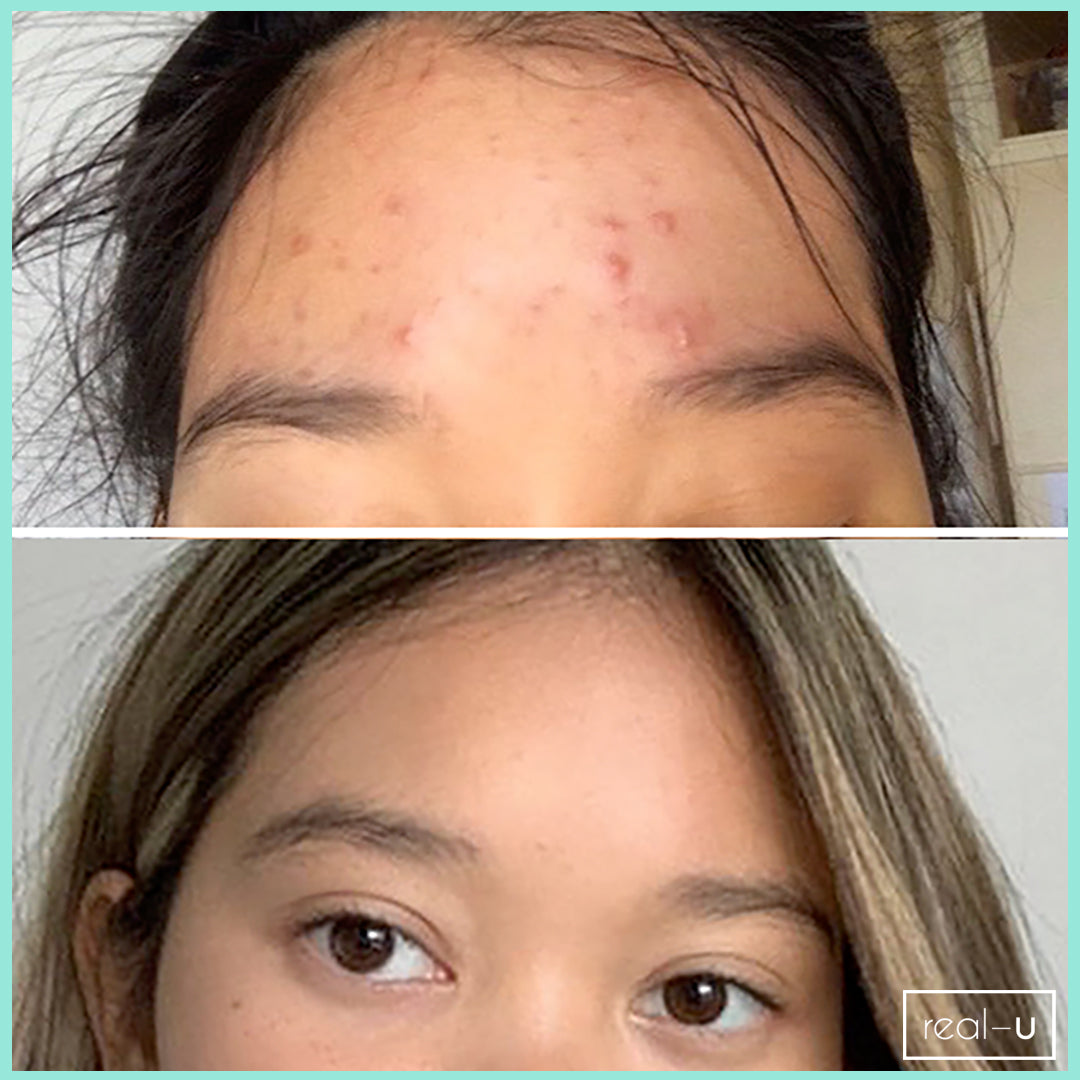
Ever heard of the term micro flora and wondered what it meant? Micro flora, microbes, bacteria, call them whatever you like, but, basically they are little organisms living on and in our bodies. There are huge numbers of micro-organisms in and on our bodies, in fact 10 times greater than the number of human cells! Much like your gut, your skin has good and bad micro-organisms (bacteria) keeping it in balance - in fact after the gut, there are more micro-organisms on the skin than anywhere else in the body.
When we hear bacteria we immediately think bad, right? Wrong!! It’s time to reset your thinking as it’s these invisible little microbes are responsible for keeping your body and your skin healthy and protected. Think of these little guys as your personalised army protecting your skin against harmful allergens, infection and pimple causing bacteria. Yes you heard me right - this little army is responsible for making sure that pimple causing bacteria (P.acnes) does not take over and play havoc with your skin. *Light bulb moment.
Recently in Paris there was an exhibition at museum de l'Homme "In my Skin” which showcased this research and explained how it directly relates to acne.
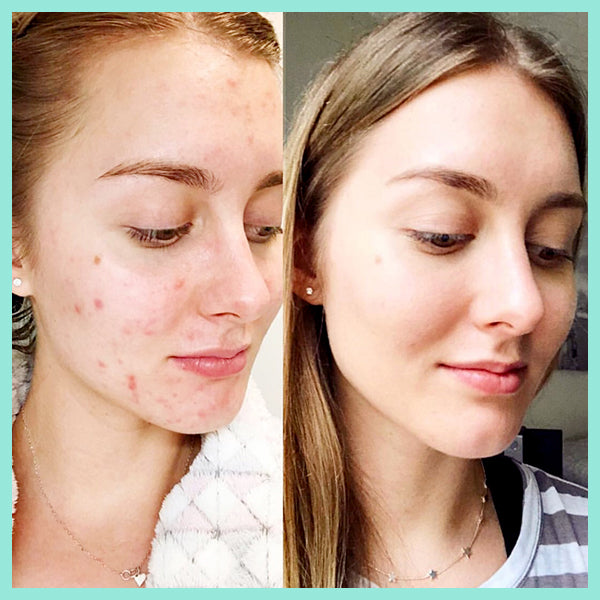
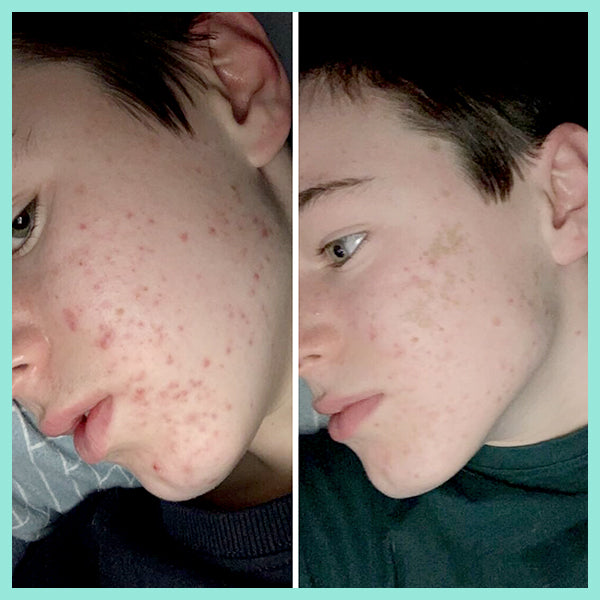
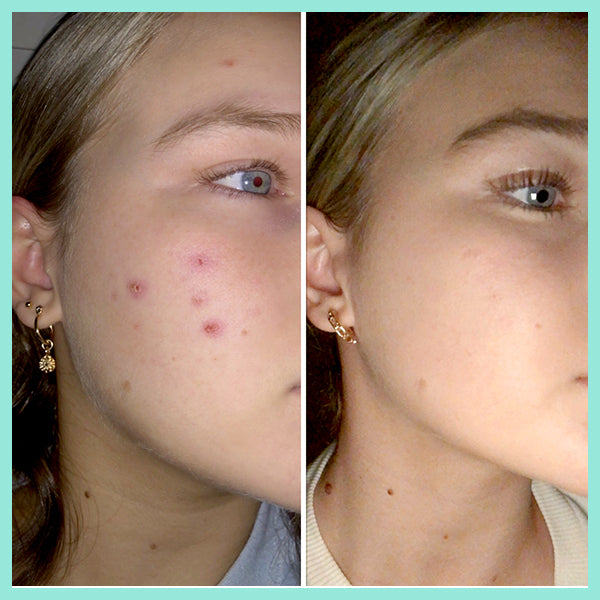
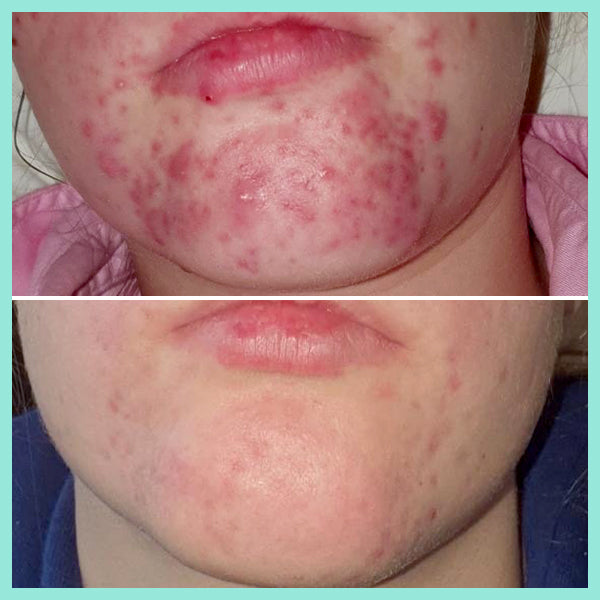
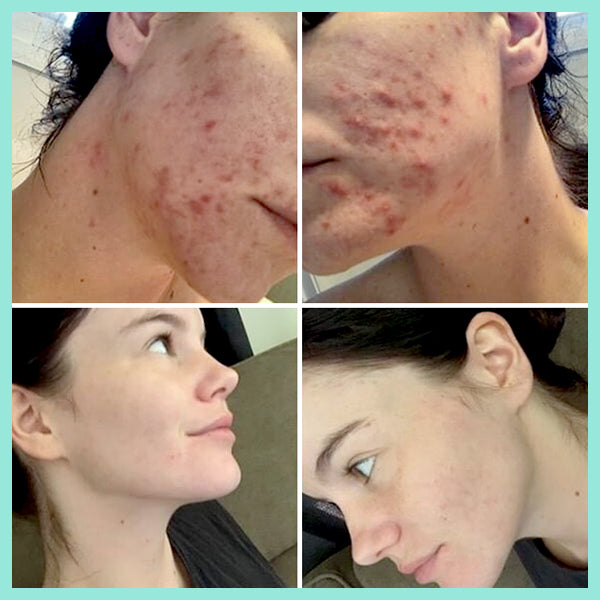
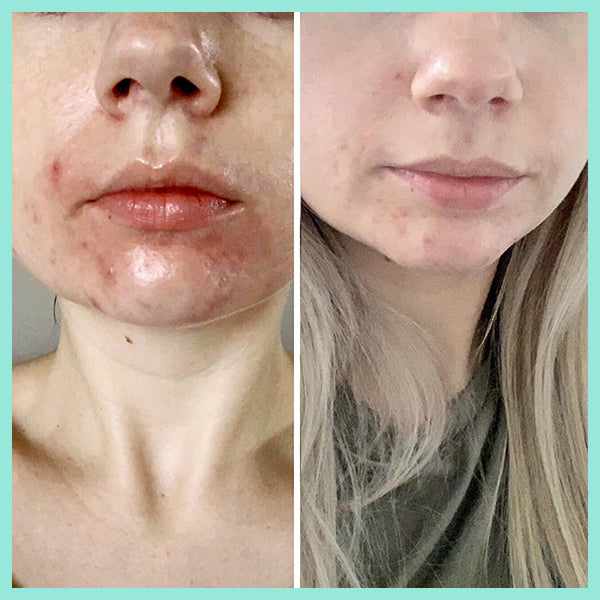
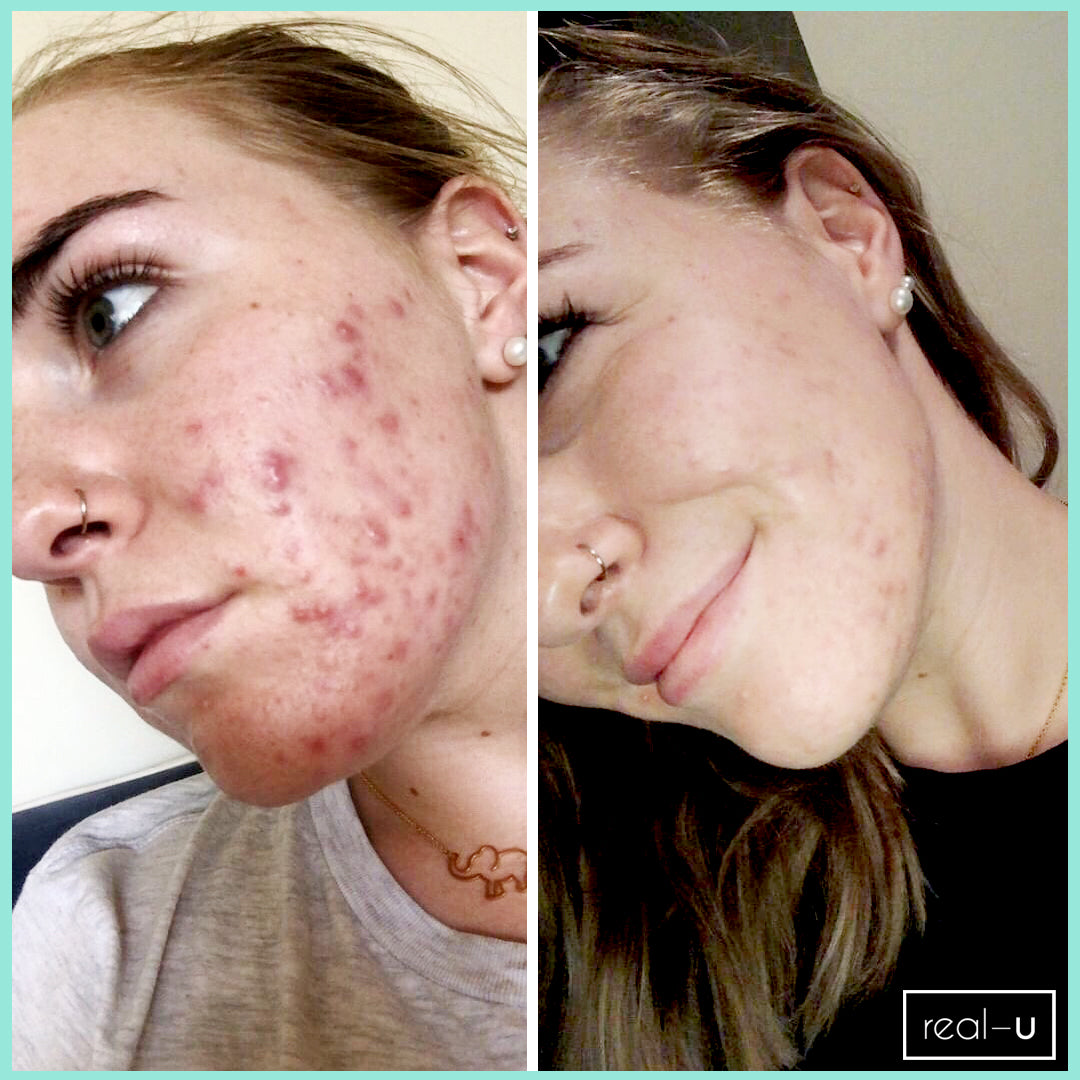
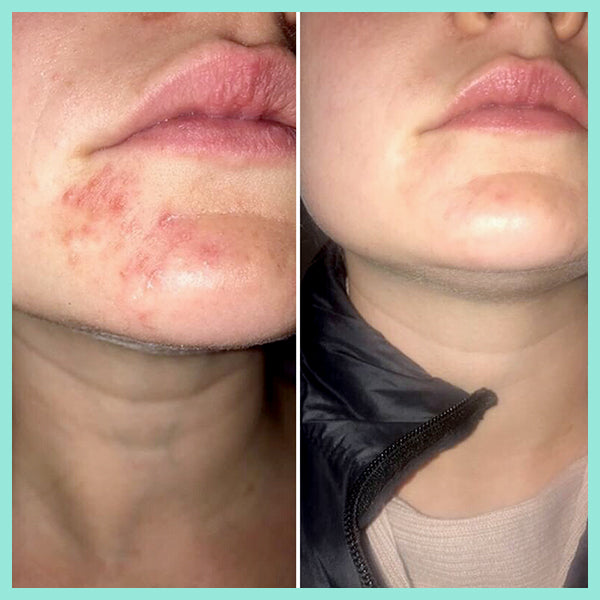
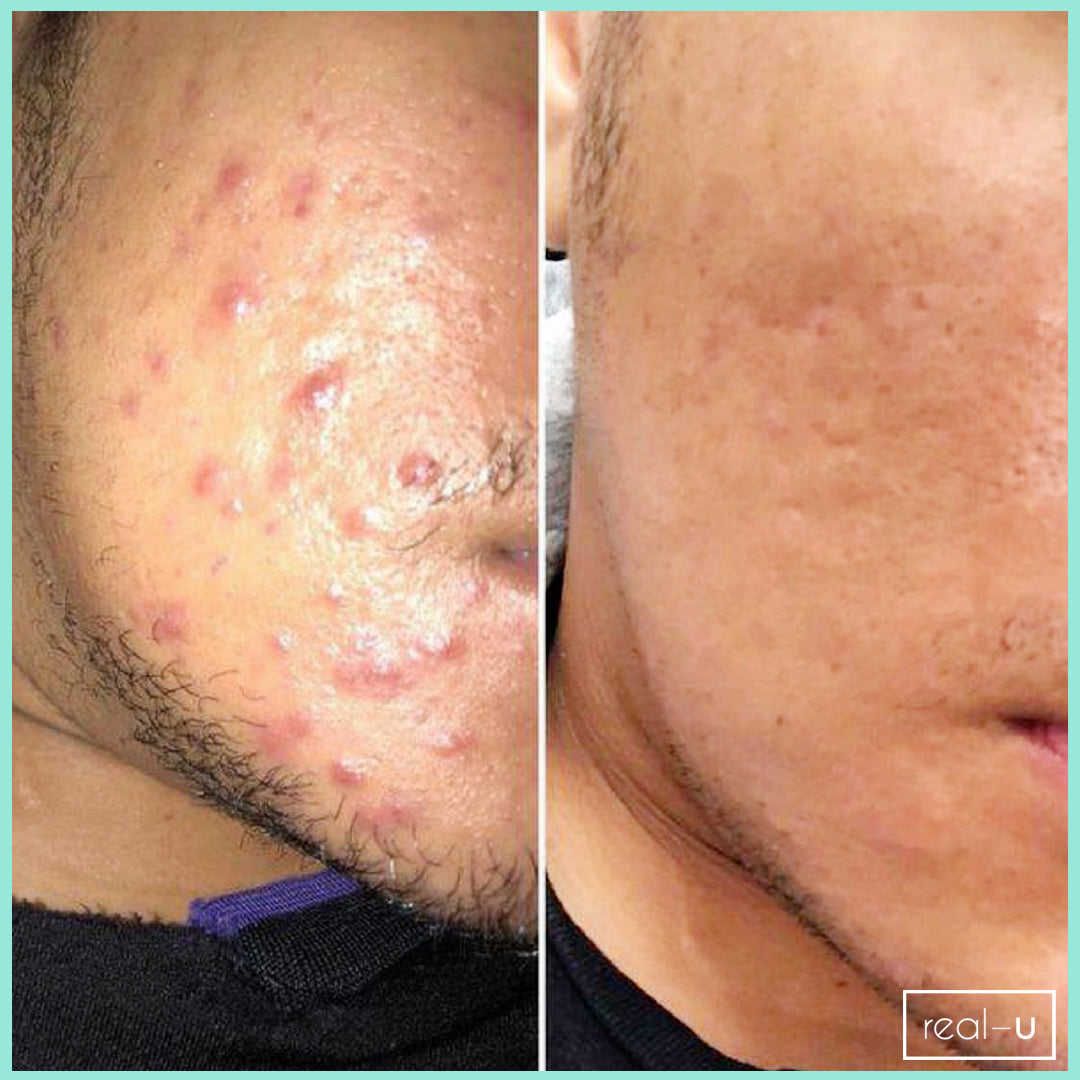
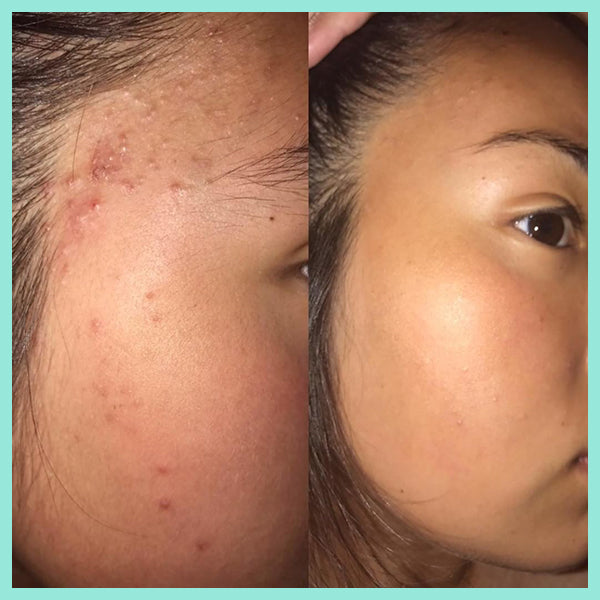
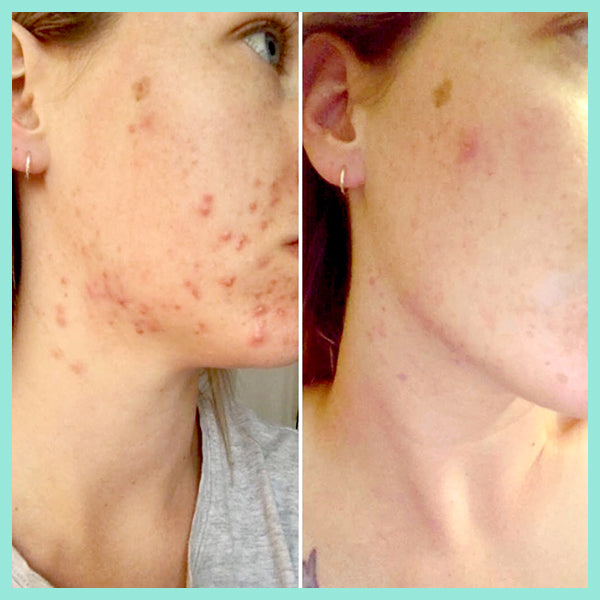
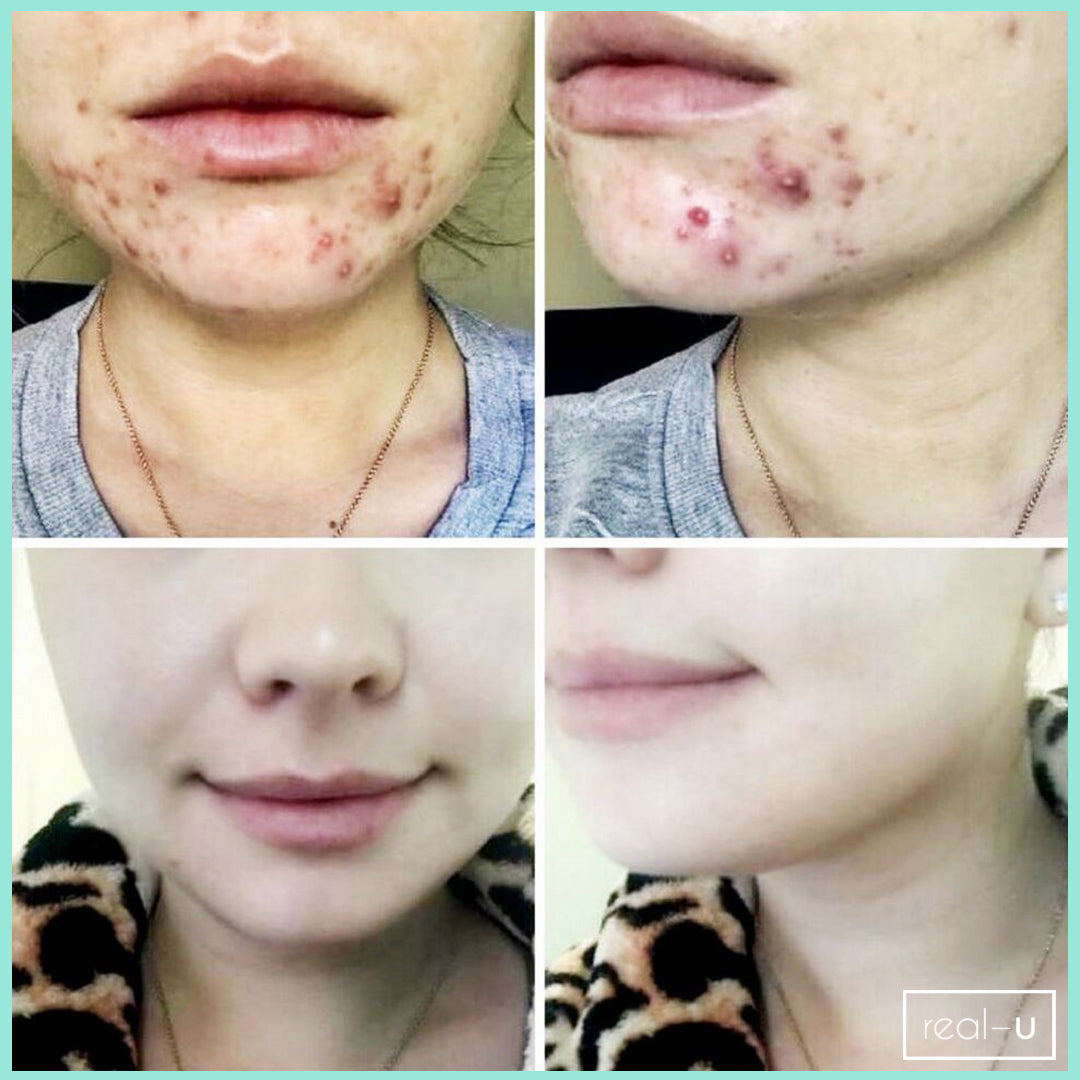
The article below "Our skin is a nest of microbes ... and that's good!" talks about how we are all born with our own unique microbes and they are as individual to each person as our fingerprints. These microbes play a massive role in protecting our skin, and are an integral part of our immune system. Factors such as diet, lifestyle, illnesses, and skincare routines all impact on the microbes on our skin. In the example of acne, if the *good* microbes are destroyed or thrown out of balance the *bad* P acnes microbes replace them - leading to inflammation and breakouts. AKA… acne.

THE BOTTOM LINE IS
You need to take care of your skin’s natural protective barrier as it delicately and effectively keeps your skin healthy and in balance. This is why it's so important NOT to use harsh, stripping products on your skin as it gives p acne causing bacteria (Propionibacterium) a chance to take over, resulting in further breakouts.
HOW REAL-U HELPS
real-u is the first acne range that supports your skin's natural protective barrier (The Acid Mantle Barrier) and actually strengthens the immunity of the skin. This is only made possible due to the breakthrough skincare technology developed by real-u. Our gentle 3 step routine is gentle on your skin, but tough on pimples.
I have translated this article into English for you to have a little read...
Our skin is a nest of microbes ... and that's good!
By Nicolas Gutierrez C.
The exhibition In my skin, at the Musée de l'Homme, invites us to discover these microorganisms that line our skin and play an essential role in immune protection.
The skin is our first protective barrier against external aggressions (pathogens, contamination, sun ...). And to ensure this protective role, the skin relies on an elite army: the cutaneous microbiota. "This microbiota is composed of bacteria, fungi and viruses that have learned to live with us from birth," says Professor Chantal Pichon, specialist in innovative therapies for skin treatment at the Center for Molecular Biophysics (CNRS-University of Paris). Orléans). And you can see this cutaneous microbiota at the exhibition In my skin, at the Musée de l'Homme, from March 13 to June 3, 2019.
Where do these microorganisms come from?
In the womb, we live in a sterile environment and we acquire our first microorganisms at birth. "Children born vaginally receive a microbiota similar to that of the mother," says Chantal Pichon, while those born by cesarean receive the microorganisms on the skin not only the mother, but also the first people who will take care of the infant. Then, this microbiota will evolve according to the environment, the age, the nutrition of the person and his state of health. "We all have about the same families of microorganisms but there is a kind of customization in their proportion. As a result, the microbiota of each individual is unique, like its fingerprints, "says the scientist.
"The microbiota of each individual is unique, like his fingerprints"
Professor Chantal Pichon of the Center for Molecular Biophysics
This microbiota also differs according to the area of the body. "The microorganisms are adapted to the characteristics of the skin: some areas are oily, like the forehead, others are wet, for example underarms or toes, and others are dry, like the forearm, describes the researcher. Fatty areas favor the microorganisms that feed on these oils and the wetlands of those that feed on our sweat. "
Team work
The cutaneous microbiota works in teams with the keratinocytes, cells of the epidermis essential for the immune defense. "These microorganisms produce antibiotics against pathogens, to prevent them from colonizing the skin," says Cécile Clavaud, skin microbiota specialist. "The pathogens are still there, but they are controlled by the microbiota-keratinocyte pair," says Chantal Pichon. "If there is an imbalance of the microbiota, these pathogens are no longer controlled and can colonize the skin, resulting in infection."
"When there is an imbalance of the microbiota, the number of" good "microorganisms decreases and pathogens settle in their place"
Cécile Clavaud, skin microbiota specialist
This can happen through a skin injury, poor nutrition or a health problem. "When there is an imbalance of the microbiota, the number of" good "microorganisms decreases and pathogens settle in their place, says Cécile Clavaud. This is for example the case of acne, where the bacterium Propionibacterium acnes replaces other benign bacteria, such as Staphylococcus epidermidis. "This change in profile of the microbiota leads to the activation of the innate immunity of the skin and the characteristic inflammation of acne.
This imbalance, known as dysbiosis, can also be caused by excessive hygiene. "Washing the excess skin can eliminate the microbiota and damage the chemical barrier of the skin, making it more sensitive," said Ms. Pichon. In addition to acne, these dysbiosis can aggravate other skin conditions, such as dandruff or inflammatory skin diseases, such as atopic dermatitis (a severe form of eczema) or psoriasis (a chronic disease of the skin). skin characterized by plaques on the body).